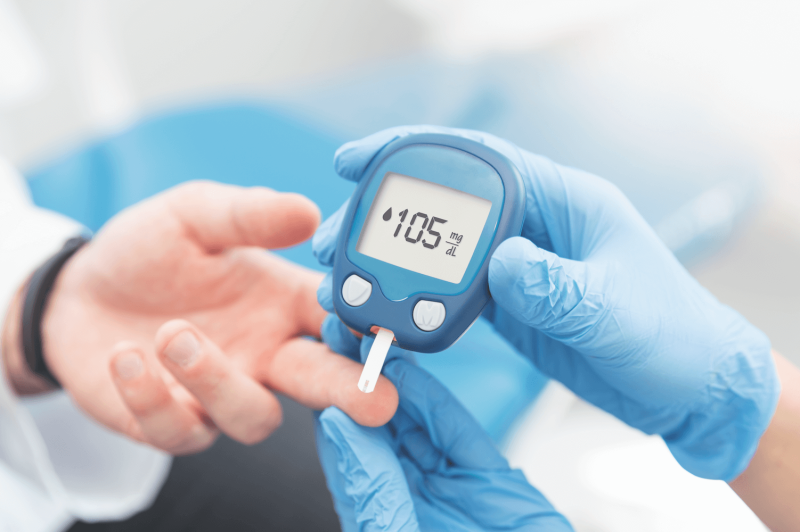
New research produces findings for a University of Virginia team studying Type 1 diabetes.
CHARLOTTESVILLE – Scientists at the University of Virginia recently completed the largest and most diverse genetic study of type 1 diabetes ever undertaken.
Through the study, researchers identified new drug targets to treat the condition, which affects 1.6 million American adults and children.
According to a 2017-18 study the Virginia Department of Health released, type 1 diabetes accounts for only five percent of all diabetes cases in the United States.
What Is Type 1 Diabetes?
You’ve probably heard of diabetes. But did you know there are two types?
Typically, people with type 2 diabetes have opportunities to rid their bodies of the disease. Oftentimes, treatment involves lifestyle changes, like diet and exercise.
For those with type 1 diabetes, there’s no cure. However, those with the disease manage their condition with insulin.
Dr. Stephen Rich, one of the study’s researchers, serves as the director of the Center for Public Health Genomics within the University of Virginia’s School of Medicine. He also serves as a professor of Public Health Sciences and a professor of Biochemistry, Microgenetics and Biology.
Rich explained that the immune system is responsible for type 1 diabetes. Normally, the immune system fights off viruses and pathogens. With type 1 diabetes, instead of attacking the virus or pathogen, the immune system attacks the body.
“There’s a whole series of autoimmune diseases. Type 1 diabetes is probably the most common, but it’s also rheumatoid arthritis, juvenile idiopathic arthritis, lupus, inflammatory bowel disease. There’s a whole series of myasthenia gravis, multiple sclerosis,” Rich said. “And in fact, these auto-immune diseases tend to cluster together. So sometimes you might have families where someone has type 1 diabetes and some family member might have an autoimmune thyroid disease like Graves’ disease or Hashimoto’s thyroiditis or something else.”
For those with type 1 diabetes, their body attacks and destroys insulin-producing beta cells.
“There is no production of insulin and because there’s no production of insulin—insulin is what translates glucose into energy for the body—so when there’s no insulin, the body attacks its own cells and systems and organs to try to get that energy,” Rich said. “And that’s why without insulin, people die.”
A Vast Study
The UVA research team doubled the participation of the prior largest type 1 diabetes study. They ultimately examined 61,427 people of Northern European, African, Asian, and Latino descent.
Rich explained how studying the tens of thousands of participants helped steer the research.
“There are a couple of approaches that we use in genetics to try to identify what are the factors in the genome that really affect risk for disease. One of those approaches is called genome-wide association scans. And so you have sites in the genome, along the entire genome,” Rich said. “We did that previously and identified about 40 regions that were important.”
The professor likened the information gleaned from the genomes to knowing that someone lives in Charlottesville, but not knowing at which house they reside.
The vast participation helped the team identify a narrower region in which to look for specific gene variants. It also gave the team significant opportunities to identify more areas of the genome out of the 186 regions.
In total, the scientists identified 78 regions on chromosomes where genes reside, which influence risk for type 1 diabetes. Of those, researchers uncovered 36 previously unknown regions.
New Findings
Researchers identified specific, naturally occurring gene variations that influence risk. They also determined how those variations act on particular types of cells. Using their findings, the team identified and prioritized potential drug targets.
Drugs targeting 12 genes identified in the diabetes study are either underway or scheduled for clinical trials for autoimmune diseases. That could accelerate the drugs’ repurposing for treating or preventing type 1 diabetes, the researchers say.
“One of the nice things that’s happened over time is that there’s been development of a whole series of drugs addressing auto-immune diseases. And so there is a drug based upon an interleukin 23 alpha gene that is available for rheumatoid arthritis, and it seems to be doing well,” Rich said. “Now before, the gene for rheumatoid arthritis – that is one of many genes, rheumatoid arthritis – but this gene was not a gene for type 1 diabetes. But with our study, we now find that it is. And so suddenly, we have drugs for other auto-immune diseases that are on the market, that are being used, that have not been used before for type 1 diabetes. Now, this points to drugs that might be able to be used.”
Rich spoke about Yale University Prof. Kevan Harold’s findings on delaying type 1 diabetes onset by almost two years.
“That suggests that there are compounds out there based on the immune system. And that’s a lot of our genes that we’re discovering, including this IL23A gene, that could be used now to slow down the progression and in fact, maybe even slow it down enough that it doesn’t happen,” Rich said. “And so if you can intervene in people who are at risk early enough, then that’s important.”
Amie Knowles reports for The Dogwood. You can reach her at amie@couriernewsroom.com